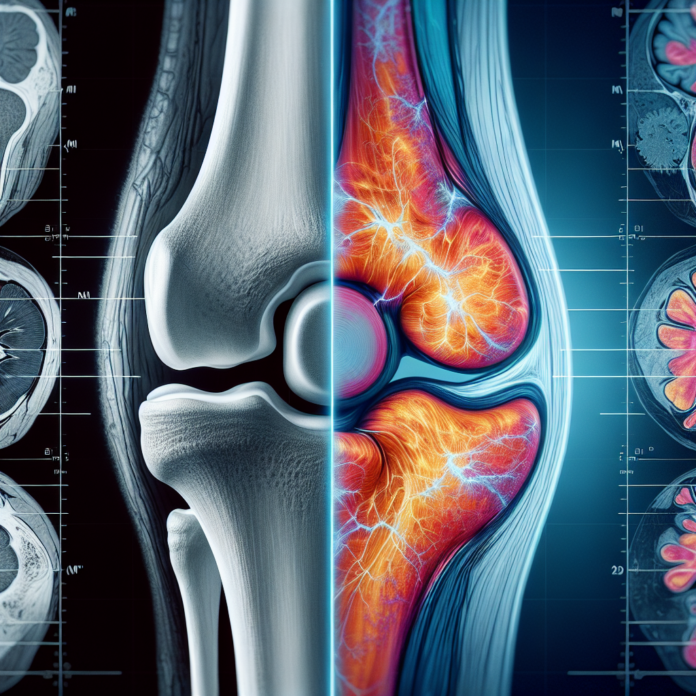
In the realm of medical diagnostics, the question of whether X-rays or MRI scans provide a clearer picture of osteoarthritis often arises. Dr. David Guyer, a renowned orthopedic surgeon and specialist in space medicine and anti-aging, tackles this inquiry head-on. He delves into the distinct advantages and limitations of each imaging modality, emphasizing that while X-rays offer detailed views of bones and the spaces between, MRIs provide insights into cartilage, ligaments, and other soft tissues. Both can reveal the presence of arthritis, albeit in different ways. However, it’s crucial to recognize that the decision for joint replacement transcends imaging alone, factoring in pain severity, prior treatments, and functional limitations. Join us as we explore these diagnostic tools, helping you fathom their roles in assessing osteoarthritis.
X-Rays: The Traditional Approach
X-rays have long been a staple in the diagnosis of osteoarthritis. They are adept at providing a clear view of the bones and the space between them. This is crucial because it allows for the identification of critical changes associated with osteoarthritis:
- Bone-on-Bone Contact: X-rays can reveal the narrowing of joint spaces, indicative of worn-out cartilage leading to bone-on-bone contact. This is one of the hallmark features of the condition.
- Bone Spurs: Osteoarthritis often leads to the formation of osteophytes, or bone spurs, which are easily identified on X-ray images.
- Weight-Bearing Views: Especially in an orthopedic office setting, weight-bearing X-rays can provide insights into the severity of arthritis by showing how the joint functions under the influence of body weight. This can sometimes give a more realistic picture of the joint’s condition compared to non-weight-bearing scans.
However, X-rays come with limitations. They do not visualize cartilage, ligaments, or other soft tissues. Thus, while they might show the consequences of cartilage loss, they do not directly display cartilage wear.
MRI: A Comprehensive Perspective
MRI scans offer a more detailed look into the internal structures of a joint. They provide a comprehensive assessment of:
- Articular Cartilage: MRIs are capable of visualizing the cartilage itself, showing thinning or the presence of divots and holes, which might not be evident on an X-ray.
- Soft Tissue Structures: Ligaments, tendons, and other soft tissues are visible in an MRI, allowing for a thorough evaluation of joint integrity and potential damage.
Despite these advantages, MRIs are not without their shortcomings. One of the primary issues is the fact that MRIs are typically conducted with the patient lying down, without the influence of body weight. This positioning may underestimate the extent of arthritis since the joint isn’t in its natural weight-bearing state.
Moreover, interpreting MRI results requires caution. The visual clarity can sometimes lead to over-diagnosis because of incidental findings that may not be clinically significant but look concerning.
The Bigger Picture in Decision-Making
It’s imperative to recognize that neither X-rays nor MRIs alone should dictate the course of treatment, especially decisions as significant as joint replacement surgery. The imaging results are just one piece of the puzzle. Additional factors include:
- Pain Severity: The level of discomfort experienced by the patient is a crucial determinant in treatment decisions. Some patients with severe radiographic changes might have minimal pain, and vice versa.
- Functional Limitations: How arthritis impacts a patient’s daily activities is a significant consideration. Can they perform their daily tasks? Are they limited in their mobility or activities they enjoy?
- Previous Treatments: The effectiveness and the range of previous treatments tried also play a role. This includes physical therapy, medications, lifestyle modifications, and less invasive interventions.
A Balanced Approach to Diagnosis
In essence, both X-rays and MRIs have their places in the diagnosis and management of osteoarthritis. They complement each other by providing a picture — albeit from different angles — of the joint status. An optimal approach typically involves using the strengths of both.
Healthcare providers should integrate imaging findings with the clinical picture, which includes patient-reported symptoms and functional status. These comprehensive evaluations lead to more personalized and effective treatment plans.
In closing, while imaging is invaluable, it is merely one aspect of a holistic strategy for managing osteoarthritis. Patients should engage in an open dialogue with their healthcare providers to understand the full spectrum of their condition and their treatment options. As Dr. Guyer underscores, the goal is to help individuals feel, look, and perform at their best, regardless of age or injury.
Explore the differences between X-rays and MRI in diagnosing osteoarthritis. Dr. David Guyer explains their respective roles and why imaging isn’t the sole determinant for treatment.