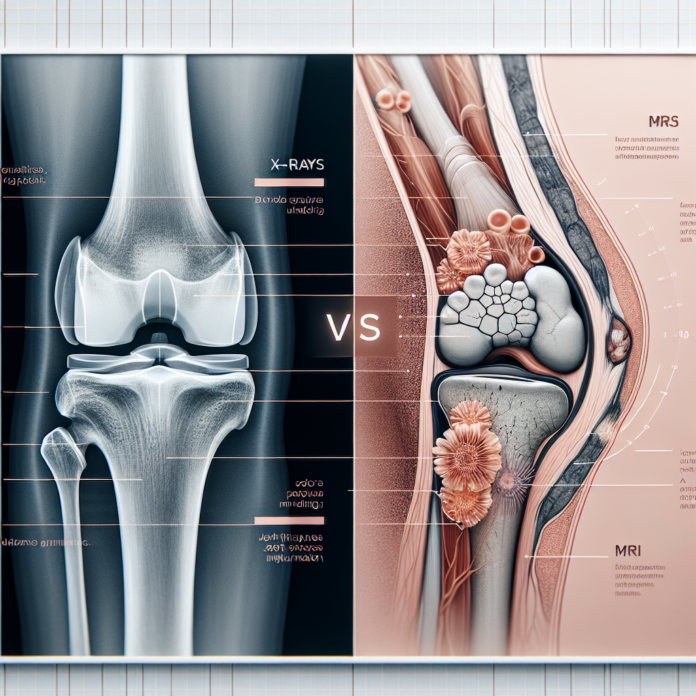
When it comes to diagnosing osteoarthritis and assessing its severity, the debate between the use of X-rays and MRI scans is crucial. Both imaging techniques serve their purpose in the medical field, yet they provide different insights into the condition of your joints. In this blog, we will delve into the advantages and limitations of X-rays and MRIs in the context of osteoarthritis diagnosis. Dr. David Guyer, a renowned orthopedic surgeon, explains how these tools can inform treatment decisions, but also emphasizes that imaging results alone do not dictate the need for surgical interventions such as joint replacements. Join us as we explore the distinct roles that each test plays in understanding osteoarthritis and making informed decisions about your health.
X-Rays: The Basics
X-rays are often the first step in diagnosing osteoarthritis. They are widely available, cost-effective, and provide a clear image of your bone structure. An X-ray will show the alignment of your bones, the space between them, and any bone spurs or calcifications that may have formed due to arthritis.
The primary advantage of using X-rays is their ability to show the extent of ‘bone-on-bone’ contact, which is a clear indicator of joint deterioration. In an orthopedic setting, weight-bearing X-rays can be especially informative. When taken while you’re standing, these images reveal how gravity and your body weight affect the joint, offering a practical perspective on how severe osteoarthritis has become. The position and motion of your knee during these scans can highlight the extent to which cartilage has worn away, and whether the meniscus — the knee’s shock absorber — is damaged.
MRI: A Deeper Insight
While X-rays provide a good overview of bone conditions, MRIs offer a more comprehensive picture by imaging soft tissues. MRI scans visualize the cartilage, tendons, ligaments, and other soft structures within the joint. For osteoarthritis, this means you can see the condition of the cartilage — whether it’s thinned or has developed holes, and compare damaged areas to those with normal cartilage thickness.
One potential drawback of MRIs, as Dr. Guyer points out, is that they don’t always reflect the real-world pressure on your joints since these scans are conducted without the impact of body weight and gravity. This can sometimes lead to an underestimation of the arthritis’ severity, providing a less dramatic picture of cartilage wear than what might be observed when you are in a standing position.
Choosing Between X-Rays and MRI
When deciding between X-rays and an MRI, the choice depends on what your healthcare provider aims to discover:
- For Bone Structure and Alignment: X-rays are preferable as they clearly show bone positioning, any ‘bone-on-bone’ erosion, and the presence of bone spurs.
- For Soft Tissue Analysis: MRIs are more suited to assess the cartilage, as well as tendons and ligaments around the joint, giving a complete view of the non-bone components.
- For a Functional View of Arthritis: Weight-bearing X-rays can offer a realistic representation of how arthritis affects daily activities.
Factors Beyond Imaging
While imaging tests are crucial in diagnosing the severity of osteoarthritis, they are not the sole determinants for opting for a joint replacement. Dr. Guyer emphasizes that the necessity for surgery also takes into account:
- Pain Severity: The level of discomfort and pain is a critical factor that could influence the decision to proceed with a joint replacement.
- Functional Limitations: How arthritis restricts your ability to perform daily activities, such as walking, climbing stairs, or participating in desired activities, plays a significant role.
- Previous Treatments: Consideration of whether non-surgical treatments — such as physical therapy, medications, or minimally invasive procedures — have been tried and their effectiveness is also crucial.
This holistic approach ensures that patients receive tailored treatments that align with their personal health goals and lifestyle needs.
Conclusion
Ultimately, both X-rays and MRI scans serve distinct purposes in the context of osteoarthritis, and each provides valuable information. X-rays are excellent tools for initial diagnoses, especially when cost and accessibility are considerations, while MRIs provide a detailed look at soft tissue health, which can be essential for a comprehensive understanding of joint health.
Understanding the pros and cons of each imaging method aids in making informed decisions about your healthcare. However, these tools are just one part of the decision-making process for treatment and potential surgery, which should always consider your pain levels, lifestyle implications, and previous treatment success. When considering these factors collectively, you and your healthcare provider can chart the best course forward in managing osteoarthritis effectively.