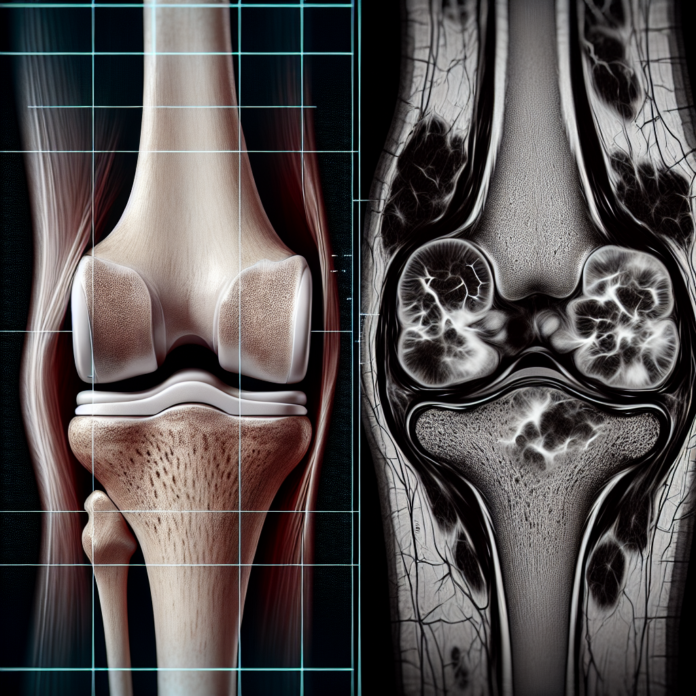
In the realm of osteoarthritis diagnosis, the choice between X-rays and MRI is a topic of much discussion and debate. Both imaging modalities offer their own sets of advantages and limitations when it comes to revealing the condition and its severity. In this blog, we will delve deeper into the pros and cons of each method as discussed by Dr. David Guyer, a triple board-certified orthopedic surgeon and specialist in space medicine, anti-aging, and regenerative medicine. Whether you’re a patient confused by conflicting medical advice or simply curious about the intricacies of osteoarthritis imaging, this exploration will provide clarity on how each tool works and what it can—and cannot—tell you about your joints. Join us as we unravel the complexities of these diagnostic tests to help you make informed decisions about your health.
X-Rays: The Traditional Approach
When you’re faced with osteoarthritis and different doctors suggest different imaging techniques, it can be perplexing. Is an X-ray sufficient, or should you undergo an MRI? To arrive at an informed decision, it’s essential to understand what each method can offer.
- Pros:
- Simplicity and Speed: X-rays are quick to perform and widely available in both hospitals and specialized orthopedic settings.
- Weight-Bearing Studies: They can be particularly insightful when conducted under weight-bearing conditions. These images give a more accurate depiction of how your bones interact under normal conditions with gravity and body weight.
- Cost-Effectiveness: X-rays are generally less expensive compared to MRIs, making them a favorable first-line diagnostic tool for both patients and healthcare systems.
- Cons:
- Limited Scope: X-rays primarily show the bones and the space between them. They don’t capture soft tissues such as cartilage, ligaments, and tendons.
- Resolution: The detail about the cartilage wear or the presence of cartilage lesions is often inferred from the decreased joint space rather than directly visualized, which can sometimes lead to under or overestimations of the actual conditions.
In summary, X-rays are effective in showing bone structures and assessing conditions like bone spurs or significant reductions in joint space indicative of “bone-on-bone” contact. However, they don’t provide the complete picture regarding soft tissues.
MRI: The Comprehensive Method
Magnetic Resonance Imaging (MRI) offers a more detailed view, particularly when it comes to the soft tissues around the joints. Here’s a closer look at what MRIs bring to the table:
- Pros:
- Detailed Visualization: MRIs can show cartilage thickness, surface integrity, and any soft tissue inflammation. This makes it superior in detecting early changes that might not yet affect the bone structure.
- Soft Tissues Insight: Beyond the bones, MRI provides a comprehensive view of the soft tissues, including ligaments, tendons, and synovial fluid.
- Non-Invasive and Not Radiation-Based: Unlike X-rays, MRI uses magnetic fields rather than ionizing radiation, which is safer for repeated use.
- Cons:
- Cost and Accessibility: MRIs are more expensive and not as ubiquitously available as X-rays. Scheduling can sometimes be delayed due to high demand in many medical facilities.
- Potential for Misleading Results: Since MRIs are performed in a non-weight-bearing position, they might underestimate the actual functional impact of joint degeneration.
- Time-Consuming: The process can take longer than an X-ray, which can be inconvenient for patients.
While MRI provides a clearer picture of the joint’s complex structures, it’s important to note that its findings must be interpreted in the context of clinical symptoms and physical examination.
A Balanced Perspective
While both X-rays and MRIs have their advantages, they should not be seen as exclusive or standalone determinants for treatment decisions. Instead, they should complement each other in a comprehensive diagnostic approach.
Considering osteoarthritis primarily affects the cartilage, an MRI can elucidate the extent of cartilage damage more accurately. Conversely, X-rays can more actively demonstrate the bone changes and joint space narrowing relevant to the condition’s progression.
It’s crucial, however, to remember that the decision to proceed with treatments such as hip or knee replacement isn’t solely dictated by imaging results. The patient’s reported pain levels, functional limitations, and response to prior treatments play equally significant roles in the decision-making process. Physicians aim to consider the entirety of the clinical picture rather than basing life-changing decisions on the black and white of an X-ray or the hues of an MRI scan.
Conclusion
For those grappling with osteoarthritis, understanding the nuances of these imaging techniques can empower you to have more informed discussions with your healthcare providers. Whether it’s choosing between X-ray and MRI, or considering their findings in treatment paths, a multi-faceted view is essential.
Ultimately, while the tools are sophisticated, they are part of a broader diagnostic toolkit that includes patient history and physical examination. The combined insights from all these aspects drive the best possible outcomes in managing osteoarthritis. By leveraging the strengths of both X-rays and MRIs, your healthcare team can guide you toward effective treatments that address your unique health needs.